
2 For MR arthrography, multiplanar small-FOV images with T1- and T2-weighting, both with fat suppression, help to delineate fluid- or contrast-filled clefts in the labrum or cartilage and paralabral cysts. Routine radial imaging to assess labral and femoral head morphology can be performed to visualize multiple segments of the labrum and articular cartilage in cross section. 1 Traditional (axial, sagittal, and coronal) planes are used, as are off-axis planes (oblique axial and oblique sagittal). Plane selection in hip imaging is challenging, as the hip joint is a highly curved structure with closely opposed cortical surfaces and relatively thin articular cartilage, making it particularly susceptible to partial volume averaging. Small slice thickness (2-3.5 mm) with minimal or no interslice gap is important for these acquisitions. Small-FOV images with fluid-sensitive sequences (proton density or T2-weighted with fat suppression) provide the best evaluation of the acetabular labrum and articular cartilage on non-arthrographic examinations. 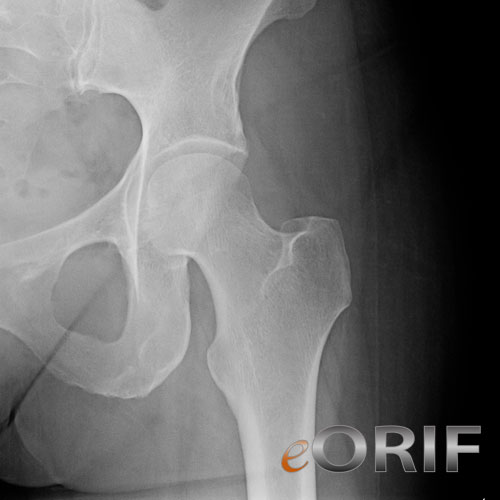
Depending on the referring clinician, dedicated imaging of the symptomatic hip may be performed only based on the clinical examination and clinical question.ĭedicated imaging of the symptomatic hip should be performed using a surface coil, such as a cardiac phased array coil, with the smallest possible FOV (15-20 cm) extending from the top of the anterior inferior iliac spine to the bottom of the lesser trochanter. For pelvic imaging, depending on patient body size, either a torso phased array coil or a larger body coil can be used. Larger slice thicknesses (5-7 mm) with small interslice gaps can be permitted for these large FOV images. Large FOV fluid-sensitive sequences, either T2-weighted with fat suppression or short tau inversion recovery (STIR), are obtained in the coronal and axial planes and are used to evaluate for fractures, fluid collections, and injuries involving tendon or muscle. Coronal T1-weighted images without fat suppression are best for revealing detailed anatomy and evaluating bone marrow and musculature. This prevents other pelvis pathology that can mimic hip pain from being overlooked. In patients with nonspecific hip pain, even unilateral symptoms, large field-of-view (FOV) images of the pelvis (30 cm or more) are commonly performed, spanning the region from the iliac crests to the level of the lesser trochanters. Imaging protocolĭedicated MRI protocols for imaging the pelvis and hip vary among institutions, but there are key elements common to most. This article provides a brief overview of considerations in tailoring protocols of the bony pelvis and hip to optimize detection of both intra- and extra-articular hip pathology, followed by a review of common labral, osteocartilaginous, and soft tissue variants that can be mistaken for true pathology. Familiarity with the spectrum of magnetic resonance imaging (MRI) appearances of the hip is necessary to recognize normal variants and distinguish them from true pathologic conditions. In addition, the capsulo labral tissues and surrounding muscles and tendons stabilize the hip, dictate its range of motion, and enhance its function. The AP of the whole pelvis (not shown on the X-rays on this page) should be fully assessed because pelvic fractures can mimic the clinical features of a hip fracture.The hip is a complex ball-and-socket joint comprising the acetabulum, proximal femur, and articular cartilage. Standard viewsĪP (Anterior-Posterior) pelvis and Lateral hip. Particular care is needed in assessing the X-ray when physical examination is limited, for example if a patient is acutely confused. Repeat X-rays, CT or MRI may be required if pain persists. In this case the X-ray may not show an obvious fracture. It is important to be aware that the common clinical signs of a shortened and externally rotated leg may be absent if the fracture is not displaced. Many hip fractures are clinically and radiologically obvious. 
Remember to assess the surrounding pelvic bonesįractures of the proximal femur or 'hip' are a common clinical occurrence in elderly, osteoporotic patients.Particular caution is required in the case of acutely confused patients.Not all hip fractures are visible on the initial X-ray and follow-up imaging may be required if concern remains.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
